Combat the Closure Epidemic
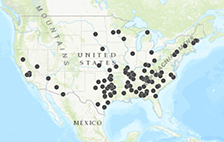
Successfully managing a rural hospital or clinic requires creative approaches to maximize potential revenue-generating opportunities. Unfortunately, there have been 94 rural hospital closings from January 2010 until December 2018, making closings one of the biggest issues to overcome in hospital management of rural facilities.
With rural populations requiring enough staff and specialists to provide care for long-term diseases and chronic illnesses, ensuring profitability for clinics and hospitals in need is essential. Rural Healthcare facilities must consider alternative revenue streams to improve purchasing and negotiation power while boosting cash flow and minimizing staff shortage issues.
Here are 5 Alternative Paths to Profitability
Common Pain Points of Rural Hospitals and Clinics

Understanding the most prevalent issues that rural hospitals and clinics face is essential to set clearly defined goals and alternative approaches for revenue generation.
Some of the most common issues among rural clinics and hospital facilities include:
-
Insufficient Patient Population:
Insufficient Patient Population:
Not enough patients to sustain profits and keep the business operating. A hospital or clinic without additional services, features, and amenities are much less likely to attract new patients or patients that require major surgery and a long-term stay.
-
Uninsured Patients:
Uninsured Patients:
With a high rate of uninsured patients it becomes increasingly difficult to generate revenue without going into the red.
-
Older/Sicker/Poorer Patient Populations:
Older/Sicker/Poorer Patient Populations:
Patients in rural areas are much more likely to struggle with chronic illness and debilitating diseases (with or without insurance). Older and poorer patients lead to an inability to generate revenue in rural locations.
-
Staff Shortages:
Staff Shortages:
A shortage of physicians and other medical staff leads to the inability to provide patient care service while generating growth and revenue.
-
Dwindling Cash Flow:
Dwindling Cash Flow:
A decreasing cash flow is one of the biggest issues faced in hospital and clinic management. Without sufficient cash available, it is difficult to implement new programs that help to sustain and expand medical facilities.
TAKE ADVANTAGE OF Grants

It is time that we start considering unconventional options to avoid the closure epidemic. The majority of rural leaders have exhausted the established approaches of cutting costs and increasing revenue. Most of the time, because of the unique challenges that rural facilities face, it is not enough to keep the doors open. Rural facilities all around the United States are talking steps to alternative solutions.
Here are the 5 Alternative Paths to Profitability
- Non-Medical Services (Wellness/Fitness Center, Healthy Caffé)
- Rural Track Residency Program
- Co-op (Better Together)
- Senior Retirement Community
- Community Health Outreach Program
Non-Medical Services (Wellness/Fitness Center, Healthy Café)

The development of non-medical services such as wellness/fitness centers, healthy cafes, and even restaurants or juice bars have a significant impact on the amount of revenue a rural hospital or clinic is able to generate. Non-medical service endeavors are optimal for rural hospitals with low patient population or clinics that are in need of additional amenities and features to attract nearby citizens.
Benefits of Non-Medical Services
Some of the most notable benefits of implementing a non-medical service for your rural clinic or hospital include:

Improved Cash Flow: Non-medical services such as a new CrossFit training class, healthy cafe, or juice bar have the ability to drastically improve a hospital’s overall cash flow. Sales from non-medical services from patients along with their relatives and visitors is a major way to increase the amount of cash you have available on-hand for future investments and ventures.
Promotes a Healthy and Thriving Community: Building onto a rural hospital or clinic promotes a healthy community in a thriving environment. Added services and amenities encourage patients to choose your hospital or facility for convenience factors, especially if they intend on a long-term stay or require additional time in the location for recovery after major surgery.
Increase in Foot Traffic: Not only do non-medical services appeal to prospective patients, but they also incentivize passersby to stop in, especially if the services are open and available to the public. Increased foot traffic is a way to reduce the overall costs of managing patients and hiring enough staff while also drastically increasing the revenue you are able to generate from third parties and outside sources. A well-received restaurant, cafe, or fitness center is a great way to promote a rural hospital or clinic and can lead to a complete turnaround when struggling to improve cash flow.
Rural Track Residency Program

Did you know that only approximately 10% of all physicians work in rural areas, despite 25% of the US population living there themselves? Implementing a rural track residency program is a way to increase the number of physicians and medical professionals working in rural communities (helping to combat staffing shortages without losing the opportunity of providing additional care to patients in need).
Benefits of a Rural Track Residency Program
Implementing a rural track residency program offers a myriad of benefits to rural clinics and hospitals. Some of the most common advantages of having a track residency program include:

Reduced Physician Shortages: Providing a track residency program that focuses on rural areas helps prevent the shortage of physicians, especially in areas of need. Family Medicine Rural Training Track Residencies: 2008-2015 Graduate Outcomes reports that over 35% of graduates of RTT residency programs were practicing in rural areas during the 7 years after graduation, which is about twice the percentage of former family medicine residents overall.
Long-Term Staffing Improvements: Studies show that physicians who train in rural areas are two to three times more likely to continue working in a rural setting and environment once they graduate and begin seeking work. When physicians are trained in rural settings, they are much more likely to feel satisfied with their placement and fulfilled with their work, even in the most rural areas throughout the country.
Motivate More Physicians to Work in Rural Areas: Attract future and current physicians to work in rural areas with a comprehensive training and recruitment plan. Hire additional staff without overspending the budget you have set in place.
-
Co-op (Better Together)

CO-OP solutions are not widely discussed in the US yet but are quickly becoming appealing to hospital administrators looking to improve purchasing and negotiation power.
Why Implement a Co-Op?
CO-OP solutions allow administrators, hospitals, physicians, vendors and insurance providers to work together, streamlining the patient management and payment process into one consolidated solution.

Improve Purchasing Power: Successful CO-OP solutions promote additional purchasing power, especially once your hospital or clinic begins attracting more patients due to the new system you have in place. Purchasing power allows for more endeavors including non-medical services and recruitment programs.
Improve Negotiation Power and Abilities: Having a CO-OP in place is a way to increase negotiation power and abilities when making decisions and improvements for rural hospitals and clinics. Other medical facilities, insurance providers, and vendor become easier to negotiate with once a CO-OP has been implemented properly.
Reduce Regional Facility Competition: Leadership has to worry less about hospital-vs.-hospital competition and health insurer rate battles. Instead the facilities are working together to overcome the common issues of their region.
Senior Retirement Community

A senior retirement community is a great way to provide for the elderly and older patients who are chronically ill. With a senior retirement community, build a positive and professional reputation in the rural area where the hospital or clinic is located.
A Benefits of a Senior Retirement Community
Some of the greatest benefits of introducing a senior retirement community affiliated with a rural clinic or hospital include:

Increase Revenue: Attract new senior patients who are in need of long-term care, even if they are not in need of emergency medical services.
Provide a Needed Service for a Local Community: Building a senior retirement community is a great way to fulfill a need, especially in rural communities while building a positive reputation among local citizens.
Garner Attention from Media Organizations: A senior retirement community is a great way to attract positive attention from media organizations such as local newspapers and news stations. Host events to boost revenue when providing additional non-medical services near the senior retirement community.
Increase Foot Traffic and Revenue with Other Non-Medical Services You Provide: Increase the amount of foot traffic in a rural hospital or clinic with a senior retirement community. Attract visitors including the relatives and friends of those who use the community themselves. Boost revenue with nearby shops, cafes, and fitness centers that are available to the public.
Community Health Outreach Program
We Care

Read missions into hospitals and clinics cost the facility more and ultimately have a negative impact on the facility’s overall bottom line. Reducing the number of readmissions, a rural clinic or hospital receives is much easier with a community health outreach program.
Benefits of a Community Health Outreach Program
According to Jencks and colleagues landmark article in 2009, 19.6% of Medicare beneficiaries were readmitted to the hospital within 30 days of discharge, and 34.0% were readmitted within 90 days. The new financial penalties for high readmission rates dictate that effort and resources need to be directed into reducing bounce backs. A successful community health outreach should have a good balance of telemedicine, home care, counselling and community partnerships.

Solving readmission struggles: Reducing readmissions is the main advantage of developing a community health outreach program for any rural hospital or clinic, regardless of its size. Community health outreach programs optimize the management of medical facilities to provide patients with all the care they require without wasting time and by having the proper resources available to offer the necessary treatment.
Discharge Faster: When patients are well-versed in post-op care and at-home care, they are much less inclined to return to an emergency room. Providing patients with extensive resources after a major operation or during their recovery is a way to minimize or eliminate wasteful spending, helping to keep rural community clinics and hospitals flourishing while generating a steady stream of revenue.
Take New Paths
Leading a rural medical facility is never an easy task, especially if you are struggling with lack of resources, staff, and revenue. With a bit of creativity and administrative flexibility, choose new paths for your Rural Healthcare Facility to boost profitability and success.

If your facility could use help implementing the solutions suggested in this article, please get in touch.
AB Med has experience with writing Grants & Proposals, evaluating Needs & Deficiencies, assisting with Planning & Implementation of new Services and Managing the everyday operations of a Medical Facility.
Most of all, AB Med is proud to support our Rural Communities!
Contact us to find out how AB Med can help you
Rural Health is our passion and focus Let’s Connect.
REFERENCES & RESOURCES
- 94 Rural Hospital Closures: January 2010 – Present http://www.shepscenter.unc.edu/programs-projects/rural-health/rural-hospital-closures/
- 41% of Rural Hospitals Operating with Negative Margins https://revcycleintelligence.com/news/41-of-rural-hospitals-operating-with-negative-margins
- NRHA – New report indicates 1 in 3 rural hospitals at risk https://www.ruralhealthweb.org/NRHA/media/Emerge_NRHA/PDFs/02-02-16PI16NRHAreleaseoniVantagestudy.pdf
- The rural hospital closure crisis: 15 key findings and trends https://www.beckershospitalreview.com/finance/the-rural-hospital-closure-crisis-15-key-findings-and-trends.html
- Rural Hospitals Face Growing Financial Trouble, Says Moody’s https://nonprofitquarterly.org/2018/09/11/rural-hospitals-face-growing-financial-trouble-says-moodys/
- Rural Health Grants https://www.aha.org/issue-landing-page/2018-02-26-rural-health-grants
- 3-minute case study: Keeping a rural hospital open https://www.athenahealth.com/insight/3-minute-case-study
- CrossFit is amassing an army of doctors trying to disrupt health care
- The role of medical education in the recruitment and retention of rural physicians https://www.tandfonline.com/doi/abs/10.1080/0142159042000192055
- Start a Rural Training Track http://wcrgme.org/start-a-rural-training-track/
- The Benefits and Challenges of CO-OPs: Where Do They Fit in Healthcare Reform? https://www.beckershospitalreview.com/finance/the-benefits-and-challenges-of-co-ops-where-do-they-fit-in-healthcare-reform.html
- Establishing a rural hospital cooperative: a case study. https://www.ncbi.nlm.nih.gov/pubmed/10117240
- Rural hospitals need new revenue sources http://alabamaliving.coop/article/rural-hospitals-need-new-revenue-sources/
- 10 Ways for Hospitals and Health Systems to Increase Profitability in 2012 https://www.beckershospitalreview.com/finance/10-ways-for-hospitals-and-health-systems-to-increase-profitability-in-2012.html
- For Hospitals and Health Systems: Strategies for Doing More with Less http://thehealthcareblog.com/blog/2014/03/28/strategies-for-doing-more-with-less/
- Reducing Hospital Readmission: Current Strategies and Future Directions
By : AB Med Healthcare Solutions






