In the recent years, suicide has reached public health crisis proportions. The rates of suicide in the developed world continue to climb. Geography, access to healthcare, unique stressors and many other factors are contributing to the disparity in numbers when quantifying how suicide affects different communities. Healthcare facilities and providers alike are at the front lines of this war. However, the ones we trust to combat suicide are not immune from its effects. Here are a few facts to help us understand and hopefully prevent suicide.
More suicides than homicides
In the United States, more than forty thousand people die annually by suicide. To put this number in perspective, 58,000 service people lost their lives during the Vietnam War (1968-1973); during the same period, 220,000 U.S. citizens lost their lives to suicide [i].
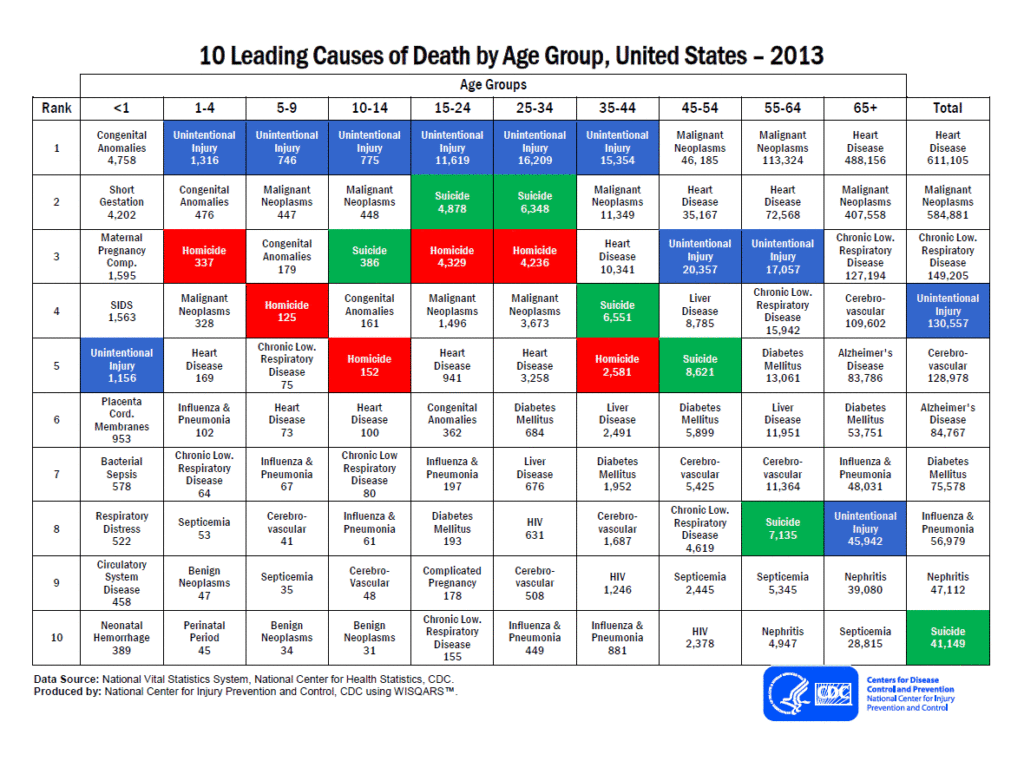
Suicide is the 10th Leading cause of death overall[ii] and according to the CDC, from 1999 through 2014; the age-adjusted suicide rate in the United States increased 24%[iii]. Lastly, suicide surpasses homicide as the leading cause of death for all age groups after the age of 10 years old. For persons aged 25–44 years, the rate of suicide was nearly twice the rate of homicide, whereas for those aged ≥65 years, the rate of suicide was nearly seven times the homicide rate[iv].
Rural Suicide

Vulnerable Populations

Despite the strengths of American Indian and Alaska Native (AI/AN) families and communities, suicide remains a devastating and all too frequent event.
The suicide rate among AI/AN has been increasing since 2003, and in 2015, AI/AN suicide rates in the 18 states participating in the National Violent Death Reporting System (NVDRS) were 21.5 per 100,000, more than 3.5 times higher than those among racial/ethnic groups with the lowest rates[vii]
Medical Providers and Departments at the front lines
Suicide of the Caregivers

An estimated 300–400 physicians die by suicide in the U.S. per year[xii]., this is on average, one doctor per day. The suicide rate among male physicians is 1.41 times higher than the general male population. And among female physicians, the relative risk is even more pronounced — 2.27 times greater than the general female population[xiii].
The available US data on nurse suicide are outdated, yet provide clues that suicide may be a risk of the nursing profession. Research is needed to assess the magnitude of nurse suicide and associated work stressors[xiv].
Prevent Suicide
Suicide is preventable. We need to re-examine how we equip our healthcare professionals to deal with this epidemic. We also need to re-examine our priorities as a society and address the stressors we put in our members. We need more research and we need to be kinder to one another.
Tools and Resources
We Care
It is not a cliché, AB Med cares about the communities and the facilities we are called to serve.
Prevention Programs
Tools
REFERENCES & RESOURCES
- World Health Organization. (2014). Preventing suicide: A global imperative. Retrieved from http://www.who.int/mental_health/suicide-prevention/world_report_2014/en/
By: Erik McLaughlin MD, MPH and Aikaterini Papadopoulou, B.Arch. Let’s Connect.

















